The Day the Peptide Market Changed
Between patients, I found myself watching something subtle but important unfold.
Not a headline. Not a dramatic announcement. No breaking news banner.
Just a quiet shift.
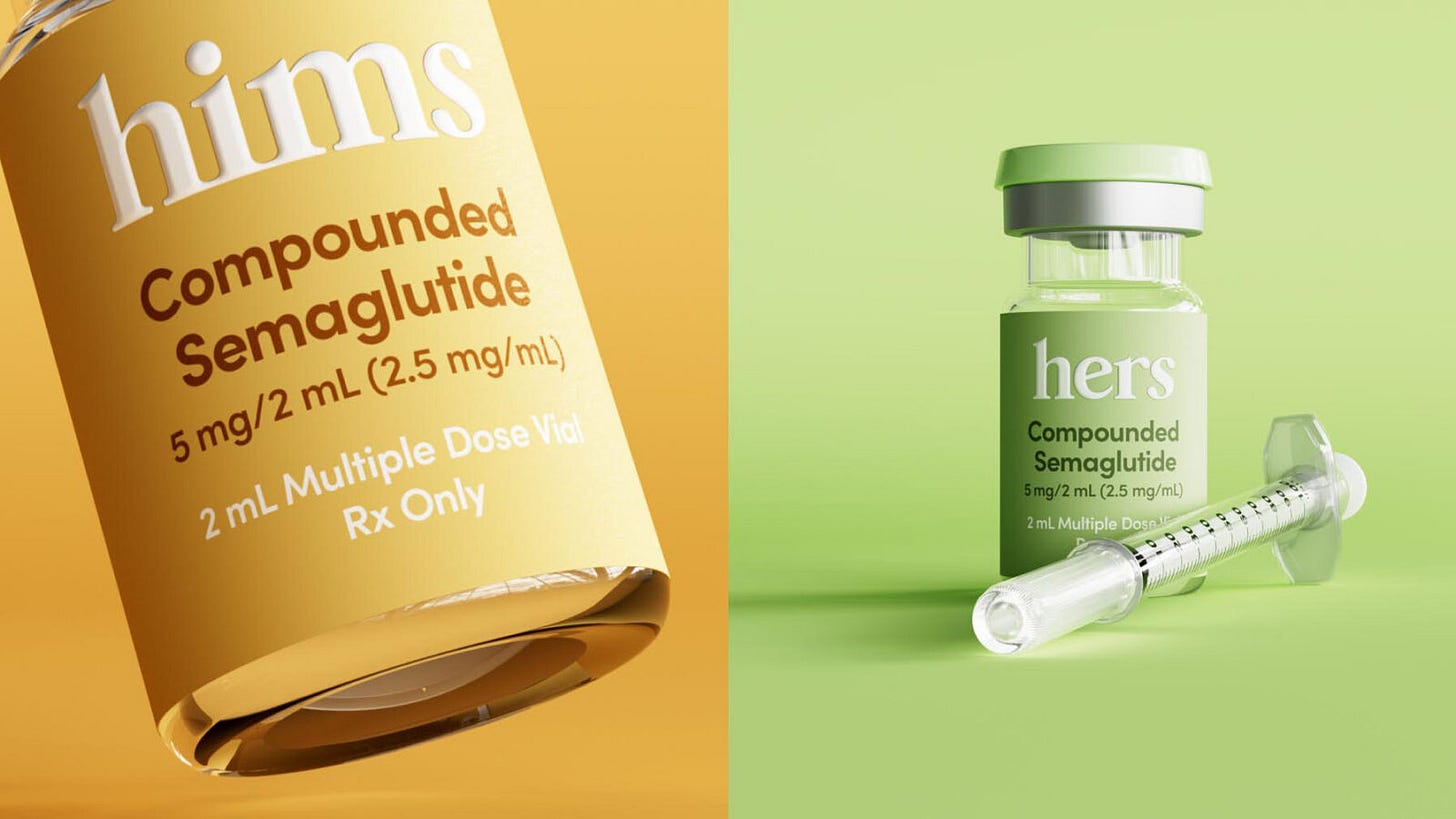
A telehealth company, HIMS, made a decision. They stopped distributing compounded GLP-1 medications and agreed to source directly from pharmaceutical manufacturers.
At first glance, it looks like a routine business adjustment. One company changing suppliers.
But it isn’t.
It’s a signal. And if you’ve been paying attention to peptides, you can feel what it means.
The ground is shifting.
But before we continue, please remember to subscribe. We couldn’t provide cutting edge Longevity Medicine insider insights without your support.
How We Got Here
For years, peptides lived in a kind of gray zone that everyone understood but no one really acknowledged.
They were labeled “research use only.” Not intended for human use.
And yet, everywhere you looked, they were being used in humans.
Physicians were using them. Clinics were building entire businesses around them. Patients were ordering them online and self-administering. Athletes were experimenting. Wellness influencers were promoting them.
At some point, the conversation moved beyond clinics and gyms.
When you start hearing about peptides in places like church, you know something has crossed a threshold.
It’s no longer niche. It’s cultural.
And once something becomes cultural, it attracts attention.
The Attention Has Arrived
What happened with HIMS is only the visible edge of something much larger that has been building for a while.
For years, the peptide world operated in a kind of tolerated ambiguity. Everyone understood the rules, but just as importantly, everyone understood how far those rules could be bent. Compounding pharmacies filled the gap between pharmaceutical pricing and patient demand. Research-use peptide companies filled the gap between regulation and access. And somewhere in between, a parallel system emerged that functioned well enough that few people questioned its durability.
But systems like that only work when no one decides to look too closely.
That condition has changed.
Pharmaceutical companies have spent the last few years quietly, and then not so quietly, reinforcing the boundaries around their products. GLP-1 medications, in particular, have become too valuable to ignore. The combination of demand, revenue, and public attention made them impossible to leave in a loosely controlled ecosystem. Patent protections were not just defended on paper, but enforced in practice. And once that process starts, it rarely stays contained to a single drug class.
At the same time, regulators have shifted from passive awareness to active scrutiny. The workaround that once felt like a clever adaptation, compounding, gray-market sourcing, research-use labeling….now looks different under that lens. What was once tolerated begins to look like circumvention. And once that reframing happens, the response tends to follow.
You can see it not just in policy, but in behavior.
Payment processors, which are often the earliest to react to regulatory risk, have begun pulling back. Access to basic financial infrastructure becomes more difficult. Transactions that were routine a year ago start failing. Companies that depended on that flow begin to feel pressure long before any formal shutdown occurs.
And then, gradually, the suppliers themselves begin to disappear.
Not all at once. Not in a dramatic collapse. But in a steady, quiet thinning of the field.
Some companies close their doors outright, deciding the risk is no longer worth the exposure. Others attempt to adapt, to find a way to remain in the market without drawing the same level of attention.
And it is in that adaptation that you see the clearest signal of all.
The phrase “research use only,” which for years served as both a disclaimer and a shield, is being replaced. Now it is “professional use only,” or “physician use only,” or some variation designed to suggest a more controlled, more legitimate pathway.
On the surface, it sounds like progress. Like a move toward responsibility.
But if you look closely, very little has actually changed.
The manufacturing is often the same.
The supply chains are the same.
The product itself is the same.
What has changed is the framing.
The same substance is now being presented through a slightly different doorway, one that implies oversight without necessarily providing it. It is an attempt to survive in an environment that is becoming less forgiving, to maintain access without triggering the same level of scrutiny.
And that is what makes this moment worth paying attention to.
Because when language starts to shift like that, when companies begin redefining what they are, rather than changing how they operate, it usually means the pressure is real.
Where the Risk Actually Lives
What has changed most is not the availability of peptides.
It’s where the risk sits.
For a long time, that risk was diffuse. It lived somewhere upstream, in manufacturing plants most people never saw, in distribution chains that were easy to ignore, TikTok firefighters, Chinese factories in legal ambiguity that allowed everyone to move forward without asking too many questions.
The peptide ecosystem behaved like a distributed system. Risk was fragmented across multiple nodes. Manufacturing variability, unclear purity, cold-chain issues, gray-market sourcing, legal ambiguity. It all existed, but no single actor fully owned it. That diffusion created psychological distance. It also left no one to be responsible for outcomes, buyer beware……
But medicine does not work that way.
Biology is not distributed. Responsibility is not distributed. Outcomes are not distributed.
They converge at the point of care.
And increasingly, it is settling on the physician.
I’ve had more than a few conversations recently with colleagues trying to make sense of this moment. There is a quiet calculation happening.
What is acceptable risk?
What is defensible?
What crosses a line that you cannot step back from?
Because once you are the one injecting a substance into a patient, the abstraction disappears. It is no longer about supply chains or regulatory language.
It is about responsibility.
What I’ve Already Seen
This is not theoretical for me. Patients are already walking in with the consequences. In fact one patient attended a conference talk solely to get my help with “detoxing” from another physician’s handiwork.
Some patients have sourced peptides themselves, often from overseas manufacturers. Others have received treatments in clinics that operate in the margins of this space.
The patterns are familiar.
Dosing that makes little physiological sense.
Products with no clear manufacturing traceability.
Complications that should not have occurred.
Situations like this stay with you.
They force you to look past the excitement around peptides and focus on something more fundamental.
How was this made?
Who verified it?
What standards were applied before it entered a human body?
Have you been harmed by peptides? Let us know!
The Question No One Wants to Ask
In most conversations about peptides, the discussion tends to move quickly to performance.
People want to know if it works. They compare protocols, dosing strategies, stacking approaches. The tone is often confident, sometimes even sophisticated, as if the only remaining question is how to optimize the outcome.
But that conversation skips over something far more fundamental.
Before you ask whether something works, you have to ask what it is.
Not in theory. Not by label. But in reality.
Was it manufactured in a way that makes it safe to put into a human body at all?
That question rarely gets the attention it deserves, in part because pharmaceutical manufacturing is invisible to most clinicians. It happens elsewhere, behind closed doors, governed by standards that are easy to reference but harder to truly understand.
But those standards are not abstract. They are concrete systems designed to remove uncertainty.
A legitimate product is not simply “pure” or “high quality” in a general sense. It has been independently verified. It has undergone sterility testing that ensures it will not introduce harm at the moment of injection. It has been produced in a facility that is inspected, documented, and accountable. It can be traced, precisely, from the batch it came from to the patient who received it. And if something goes wrong, there is a mechanism to investigate, respond, and correct.
That is what defines medicine at a systems level.
When those elements are in place, you are participating in a structure that is designed to protect both the patient and the physician. There is a chain of accountability that extends beyond the moment of care.
When they are absent, that structure disappears.
And what replaces it is not a lighter version of medicine. It is something else entirely.
It may look similar on the surface. The vial may have a label. The protocol may sound familiar. The intended effect may even be the same.
But without the underlying system, you are no longer practicing within medicine as it was built.
You are operating outside of it.
The Tension We Are Now Facing
There is an uncomfortable truth sitting underneath all of this, and most people in the space can feel it even if they don’t say it out loud.
Many of these peptides likely do have real clinical value. Not theoretical value. Not hype-driven value. Real, physiologic impact.
You see it in practice. A patient on a GLP-1 loses weight, their insulin resistance improves, inflammation markers come down, joints feel better, sleep improves. That is not subtle.
You see it with certain mitochondrial peptides like SS-31, where patients with fatigue or post-viral syndromes describe a level of energy recovery that is difficult to dismiss as placebo.
You see it with growth hormone secretagogues, where body composition shifts, recovery improves, and older patients regain some functional reserve.
So both patients and physicians are not imagining this. They are responding to signals that appear to be real. That is what makes this complicated.
Because at the same time, the pathway to access many of these compounds is anything but clean.
Take the GLP-1 story. Demand exploded faster than the pharmaceutical supply could keep up. Compounding pharmacies stepped in to fill the gap. Patients who could not afford or access branded medications suddenly had another option. For a while, it felt like a solution.
Until it didn’t.
Questions emerged about consistency, dosing accuracy, sourcing of raw materials. Regulators stepped in. Companies pulled back. What looked like expanded access began to look like a temporary workaround.
Or consider the research peptide market. A patient orders a vial online labeled “for research use only.” The same peptide might be discussed in clinical circles, presented at conferences, even used quietly in some practices. But the product itself has no guaranteed sterility, no verified manufacturing standards, no clear chain of custody.
One version of that molecule may be effective. Another may be degraded. Another may be contaminated. From the outside, they look identical. From the inside, they are not.
That is the tension.
On one side, there is restriction. Regulatory frameworks that move slowly, pharmaceutical pipelines that take years, pricing structures that put certain therapies out of reach for many patients.
On the other side, there is the workaround. Faster access, lower cost, broader availability, but with a level of uncertainty that is often underestimated.
Neither side is fully satisfying.
Strict restriction delays access to therapies that may genuinely help people.
Unregulated access exposes patients to variability and risk that is difficult to quantify until something goes wrong.
So clinicians and patients find themselves in the middle, trying to navigate a system that does not yet have a clean path forward.
And that middle ground is where the hardest decisions are being made right now.
What Happens Next
When systems reach this point, they do not stay static.
They correct.
I expect more suppliers to close. More enforcement actions. More friction in payment and distribution. And inevitably, higher prices for anything that remains available through legitimate channels.
But the more important shift will not be economic.
It will be professional. Physicians will be forced to decide where they stand.
Some will continue to operate in the gray, accepting the risk as part of their model.
Others will step back, waiting for clearer pathways and better infrastructure.
Most will feel the weight of the decision.
Where I Stand
For me, the line is simple.
If a product does not meet the basic standards of pharmaceutical manufacturing, I do not use it in a patient.
That is not a moral stance. It is not about being conservative or progressive. It is a practical decision rooted in how medicine actually works when things go right and, more importantly, when they go wrong.
Because when something goes wrong, the question is never just what happened.
The question is what system did you rely on when you made that decision.
Medicine is built on trust, but that trust is often misunderstood.
People think of trust as outcome-based. Did the patient get better? Did the therapy work?
But in reality, trust is process-based.
It is built on the invisible infrastructure behind every decision:
How was this made?
Who verified it?
What standards were applied before it reached my hands?
If there is a complication, can I trace it, explain it, and respond to it?
When those answers are clear, medicine functions the way it is supposed to.
When they are not, you are no longer standing on a system. You are standing on an assumption.
And assumptions fail quietly until they don’t.
Is your doctor peptide curious? Please share this with them.
I’ve had patients come in after receiving therapies elsewhere where, on paper, everything looked reasonable. The molecule made sense. The protocol was familiar. The intent was appropriate.
But when you start asking basic questions about the product itself, the foundation disappears.
Where was it manufactured?
Was it sterile?
Was it independently tested?
Can anyone verify the batch?
And suddenly, no one can give a clear answer.
At that point, the conversation shifts. It is no longer about optimizing a protocol.
It is about unwinding uncertainty.
So for physicians operating in this space, the guidance is straightforward, even if it is not always easy.
Before you consider mechanism, before you consider efficacy, before you consider demand, ask:
Does this product meet the minimum standards of medicine as a system?
That means:
You know where it was manufactured
You know the facility is inspected and accountable
You have documentation of sterility and purity
There is independent verification, not just a manufacturer’s claim
There is a chain of custody from production to patient
There is a mechanism for reporting and responding to adverse events
If those elements are not present, you are not working within a medical framework.
You are improvising.
The next layer is documentation and defensibility.
If you choose to use a therapy, you should be able to explain:
Why this product, specifically, was selected
What standards it met
What alternatives were considered
What risks were discussed with the patient
Not in vague terms. In precise, defensible language.
Because increasingly, that is the standard that will be applied.
There is also a responsibility to recalibrate how we talk to patients.
Patients are often focused on access and results. They hear about peptides from friends, from online forums, from social media. By the time they walk into your office, they are not asking if something is appropriate. They are asking how to get it.
Part of the physician’s role now is to reframe that conversation.
Not by dismissing the therapy outright, but by introducing a level of rigor that most patients have never been exposed to.
Explaining that:
Not all versions of the same molecule are equivalent
Manufacturing matters as much as mechanism
Safety is not just about the peptide, but about how it is produced
When patients understand that, most of them recalibrate quickly.
Because what they actually want is not just access.
They want reliable access.
Finally, there is the discipline of restraint.
There will be cases where a therapy is promising, where the mechanism makes sense, where early data is encouraging, and where patient demand is high.
And the correct answer may still be:
Not yet.
Not because the therapy is invalid, but because the system around it is not ready.
That is one of the hardest positions to hold in modern medicine, especially in a field moving as quickly as longevity and peptide therapeutics.
But it is also one of the most important.
If the foundation is solid, you can build something meaningful on top of it.
If it is not, everything else becomes secondary.
And over time, that difference becomes very clear—not just in outcomes, but in who is still standing when the system tightens.
That is where we are heading.
The Shift That Matters
The peptide market is not disappearing.
But the version of it that operated quietly in the background, tolerated because it was useful and largely unexamined, is coming to an end.
What replaces it will look different.
More structured.
More accountable.
And in the long run, that may not be a loss.
Because medicine, at its best, is not about access alone.
It is about access that you can stand behind.
Here’s To A Life Well Lived.
-Dr M